HPV virus infection is a virus that can cause genital warts and cervical cancer. It can be transmitted by skin-to-skin contact, although it is usually transmitted by sexual contact, it has also been shown that it can be transmitted by direct skin contact.
Table of Contents
What is HPV Virus Infection?
human papillomavirus; HPV , in other words , is a sexually transmitted virus that can cause genital, anal, oral and some parts of the body to form warts (condyloma) and cervical cancer. Most infected people do not have any symptoms or complaints, and the virus clears from the body within a year or two. In 10-20% of women who are contagious, the virus cannot be cleared from the body and causes complaints.
There are more than 100 variants of the human papillomavirus. Of these, types 6 and 11 cause genital warts and condylomas. It has been proven that other types such as Type 31, 33, 45 and 58, especially Type 16 and 18, play a role in cervical cancer.
How is it found?
How can it be transmitted by adults ?Should be known and necessary precautions should be taken accordingly. Scientifically, the reasons for the transmission of the virus;
- with virus with someone You can catch the virus by having vaginal, anal, or oral sex. It is most commonly spread during vaginal or anal sex. It can pass even if an infected person has no signs or symptoms.
- The World Health Organization states that human papilloma infection is very common because penetrative explained that it can spread without intercourse. This means that it can be transmitted simply by skin-to-skin contact.
- You can be infected with the virus without being sexually active – it is possible to become infected with the Human papillomavirus without having sexual intercourse, as this virus spreads easily through skin-to-skin contact. Prolonged contact with infected skin, such as holding hands, can transmit the virus.
Most cases of the virus clear up within 1 to 2 years as the immune system fights and clears the virus from the body. After that, the virus disappears and cannot be transmitted to others. In extreme cases, the transmitted virus may lie dormant in the body for years or even decades.
HPV Transmission Options
HPV transmission options are classified according to their mode of transmission. According to this;
Contamination from the External Surface
The infection can be detected in inanimate objects such as clothing or environmental surfaces. However, transmission is not known to occur in this way.
Auto-Inoculation Contamination
Co-assisted transmission, autoinoculation or transmission from inanimate objects shortly after sexual intercourse may explain concomitant (simultaneous) genital and anal infections.
Vertical Contamination
Vertical transmission of HPV from mother to fetus is known to occur. Indeed, up to 80% of newborns born to women with genital warts have detectable virus DNA in their nasopharyngeal aspirates or oral mucosa, and this may persist for months or years.
Is HPV Transmission Possible Without Sexual Intercourse?
HPV is transmitted through skin-to-skin contact, not through bodily fluids such as semen or saliva. This happens most easily through sexual contact, such as vaginal, anal, and oral sex. However, anyMucosa It can also happen if it comes in contact with membranes (such as the mouth, lips, anus, and parts of the genitals) or skin bruises. Condoms, when used correctly, reduce the risk of transmission. This protection is not one hundred percent, but it does have an effect. This is because the virus peni is present in the skin.
How Long Does the HPV Virus Appear?
It shows symptoms between 2 weeks and 2 years after being infected with the HPV virus . In some cases, the virus is eliminated from the body without any symptoms during this period. In some cases, during this period, anal, oral, vaginal warts and virus symptoms may occur.
Who Gets HPV?
Anyone who is sexually active can get HPV, even if you’ve only had sex with one person. You can still develop symptoms years after having sex with an infected person. But there are also people and conditions at high risk of HPV . Conditions at risk for HPV;
- Polygamy
- unprotected intercourse
- Early sexual intercourse
- Cigarette consumption
- low immunity
- chronic diseases
- It can be explained as not performing routine gynecological examinations for women.
What Are the Symptoms of HPV Virus?
“How does the virus show symptoms?” “What are the symptoms?” We will answer your questions. Low-risk types rarely turn into cancer but can cause symptoms such as genital warts around the genitals and anus. However, these symptoms do not always appear. For example, they can occur in the anus, vagina, or cervix. High risk may not show any symptoms. Therefore, HPV virus symptoms may not always be followed easily.
What is Genital Wart?
Condyloma acuminata refers to anogenital warts caused by the human papilloma virus. The most common types of viruses that cause anogenital warts are 6 and 11. It is a double-stranded DNA virus that spreads primarily through sexual contact. Condylomas or genital warts are pink-brown cauliflower-shaped formations on the skin that appear raised from the surface. Usually types 6 and 11of the types they originate. Although it can be seen in both sexes, women are more often affected. Genital warts usually do not cause any complaints, however, they can bleed with friction and be cosmetically uncomfortable.
There are many medical and surgical methods with a similar success rate in the treatment of warts. The desired treatment can be selected according to the location of the warts and the patient’s characteristics.
How Are Genital Warts Transmitted?
The answer to the question of how genital warts are transmitted ; You get it by touching your genitals with the genitals of someone else who has the virus. The virus may be present on the skin but true warts cannot be seen. You can get warts even if you use a condom, because condom It does not cover the entire genital skin. Direct contact with the area of condyloma will increase the risk of genital wart transmission .
What are the Symptoms of Genital Warts?
In women , genital warts appear in and around the vagina or anus, or on the cervix. They can be very small or appear in large clusters. They can be described as structures resembling cauliflower. They can be reddish in color or white. Sometimes you can have genital warts but show no symptoms.
What are HPV Types?
In this article, we will answer the question of what are the HPV types and which types cause which diseases. There are more than 200 identified strains of human papillomavirus. High-risk human papillomavirus strains include 16 and 18, which cause about 70% of cervical cancers. Other high-risk human papillomaviruses include 31, 33, 45, 52, 58 and a few more. Low-risk virus strains such as 6 and 11 cause about 90% of genital warts, which rarely turn into cancer.
6 and 11 are low-risk types. They are linked to about 90 percent of genital warts. Type 11 can also cause changes in the cervix. Genital warts look like cauliflower-shaped bumps on your genitals.
They usually appear a few weeks or months after the sexual partner has been exposed. Getting vaccinated can help prevent HPV 6. The vaccine also provides protection against type 11. Gardasil has shown an 89 to 99 percent improvement in protection against types 6 and 11 in clinical trials.Activity showed.
It is recommended that vaccines be received before becoming sexually active, as the vaccine cannot protect against a strain a person has already been exposed to. If you get a 6 or 11 diagnosis, your doctor may prescribe medications such as imiquimod or podofilox (Condylox). These are topical medications that destroy genital wart tissue. You can apply these drugs directly to your genital warts.
Which Type Causes Cancer?
The 14 most cancer-causing types include types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66 and 68. Cancer together accounts for approximately 70% of invasive cervical cancers. However, not all infections with Type 16 or 18 turn into cancer.
What Types Cause Genital Warts?
Warts may appear in the mouth and throat. Two types of HPV, types 6 and 11, cause 90 percent of these warts. Only 1 percent of sexually active people have noticeable genital warts that require treatment to prevent them from spreading to other genitals and sexual partners.
Which Types Are Self-Expelled?
In most cases, your body can produce antibodies to the virus and clear the virus within one to two years. Most HPV types go away permanently without treatment. Therefore, it is not unusual to completely shut down and clear the virus before you know you have it.
Does Each Type Show Symptoms?
In the majority of patients, human papillomavirus does not show any symptoms and can be cleared within a few years without any changes in the body.
How is HPV Diagnosed?
There is no test for the diagnosis of HPV to find out if a person is infected. Also, there is no approved test to find the virus in the mouth or throat. Can be used to screen for cervical cancer tests has. These tests are only recommended for screening in women age 30 and older. Tests are not recommended to screen men, adolescents, or women under 30
Most people do not know they are infected and therefore never develop symptoms or health problems. Some people find out they are infected when they show signs of genital warts. Women can find out they have it when they get an abnormal Pap test result (during cervical cancer screening). Others may find out when they develop more serious problems, such as cancer.
Diagnosis in Young Girls
Teenage girls do not need to have a Pap smear unless their doctor thinks there is a problem. Once a girl turns 21, she should start getting regular Pap smears as a way to monitor her health. Women in their 20s with normal Pap smear results should get tested every 3 years.
Smear Disorders & HPV Screening
As a result of the smear and screening performed for cervical cancer screening, changes due to infection can be detected. The most common of these are ASCUS, LSIL, HSIL and AGUS. If detected as a result of screening or in case of a smear disorder, these findings may need to be evaluated under colposcopy by a gynecological oncology surgeon.
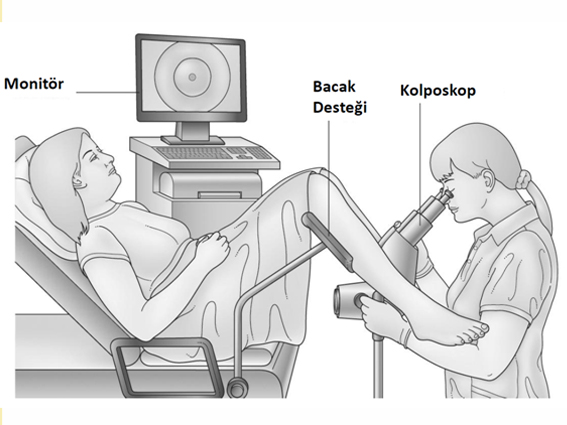
colposcopy
Cervical smear (smear) or abnormality in one of the HPV tests for cervical cancer in case of The recommended application is Colposcopy. Thanks to colposcopy , the cervix can be examined in detail with a magnifying glass and a biopsy can be taken from the cervix if necessary. Colposcopy is a procedure that can usually be performed in office conditions without the need for any anesthesia, however, it can also be performed under anesthesia according to the needs of the patients.
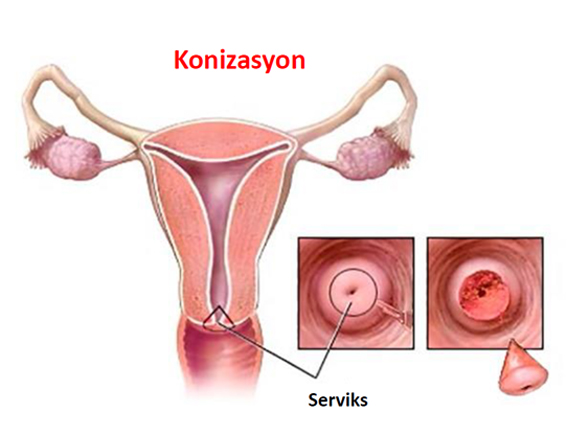
LEEP and Conization
In case of abnormality in one of the cervical smears (smear) or HPV tests performed for cervical cancer, another recommended application is LEEP and Conization. With this procedure, HPV diagnosis and treatment is carried out.
Depending on the infection, some changes may occur in the cervix. These can be detected by smear test or human papilloma virus test. If a high-grade lesion (HSIL) is detected by cervical biopsy performed with LEEP and conization, your physician can apply this procedure to your cervix both to understand the limits of this disease and to understand whether there is cancer and to treat it. More clear information about the disease is obtained by sending the piece taken to the pathology.
You can reach the detailed article I wrote about the LEEP procedure, LEEP risks, pre-procedure preparation and post-treatment at https://drdermanbasaran.com/leep-nedir/ .
HPV Vaccines
At the beginning of the 2000s, vaccines against human papillomavirus were produced, and currently, there are two types of human papilloma virus vaccines available in our country as well. HPV vaccine ; It is Gardasil 4 and Cervaix. Studies have shown that;
- Vaccines are very effective in preventing viral infections and precancerous changes in the cervix.
- Vaccination of the virus reduces the appearance of genital warts.
- This reduces the risk of virus-related cancers.
- The ideal vaccination age can be summarized as 12-18 years.
What is the HPV Vaccine?
The HPV vaccine helps protect you against certain types that can cause cancer or genital warts. Also known by the brand name Gardasil 9, the HPV vaccine protects against: HPV types 16 and 18 – the 2 types that cause 80% of cervical cancer cases. HPV types 6 and 11 cause 90% of genital warts cases. The vaccine also covers 5 other types that can cause cancer of the cervix, anus, vulva/vagina, penis or throat. (types 31, 33, 45, 52 and 58).
How Many Doses of HPV Vaccine Are Used?
The HPV vaccine is given as a series of vaccines. There are 3 separate vaccines available for people aged 15-45 years. The second dose is given 2 months after the first dose, and the third dose 4 months after the second dose. So, it takes about 6 months to do all 3 doses in total. For people 9-14 years old, you only need 2 doses. The second dose is given 6 months after the first dose.
At What Age Should The HPV Vaccine Be Preferred?
All people between the ages of 9 and 45 can be vaccinated to protect against genital warts and/or the different types of HPV that can cause cancer. It is recommended that children receive the vaccine at age 11 or 12 so they are fully protected years before they become sexually active. But whatever your age, talk to your nurse or doctor to find out if the vaccine would benefit you.
HPV Treatment Methods
There is no proven treatment for HPV treatment methods . Most infections do not cause any problems and are cleared by your body within 2 years. Treatment is necessary if it causes problems such as genital warts or changes in the cells of the cervix. There is no current cure for HPV – the human papillomavirus is the name given to a group of more than 100 related viruses, the most common sexually transmitted disease worldwide. However, there are treatments for warts caused by the virus.
Medication
Genital wart treatments, over-the-counter salicylic acid products, can treat common warts. However, do not use these products on warts in the genital area. For some patients, the doctor may prescribe one of the following medications:
- imiquimod (Aldara, Zyclara)
- podofilox (Condylox)
- trichloroacetic acid
- podophylline
Without consulting your doctor, the necessary diagnosis and suitable You should not apply the drugs you bought from the pharmacy to your genital area without learning the treatment method.
cautery treatment
Genital wart treatment methods include electrocautery, genital warts around the penis, vulva or anus with a low-voltage electric destroys it by burning it with the probe. Electrocautery is usually done in a doctor’s office or a clinic. An injection of a numbing drug (local anesthetic) is often used for pain control. Depending on the number of warts to be removed or destroyed, a drug that causes unconsciousness (general anesthetic) can be used.
Laser Therapy
HPV treatment methods can use a laser to remove genital warts. Laser surgery can be done in a doctor’s office or clinic, hospital, or outpatient surgery center. Local or general anesthetic can be used depending on the number of warts to be removed or the size of the area to be treated. For women, abnormal cervical cell changes caused by the virus will be managed differently from genital warts caused by the virus. Your doctor may prescribe certain medications, such as laser surgery operation suggest types.
Cryotherapy Treatment
Genital wart treatment methods cryotherapy (cryotherapy) destroys genital warts by freezing them with liquid nitrogen. A doctor applies liquid nitrogen around the wart. First, the tissue is frozen with liquid nitrogen. The tissue is then allowed to dissolve.
To Whom Are HPV Treatment Methods Applied?
There is no cure for the virus itself. However, there are treatments for the health problems that HPV can cause: Genital warts can be treated by your healthcare provider or with prescription medications. If left untreated, genital warts may disappear, stay the same, or grow in size or number. If patients have an allergy to one of the treatment methods or if a problem has been detected in previous applications, that method should not be used. Because there is no treatment for HPV virus, thousands of people die every year. Therefore, people should take the necessary precautions to avoid contact with this virus.
